What Is Skin Surveillance?
Skin surveillance is a structured process used in occupational health to monitor an employee’s skin condition when they are exposed to workplace hazards. It focuses on early identification of changes such as dryness, redness, itching, or cracking before they develop into occupational dermatitis.
Unlike general health checks, skin surveillance is risk-based; it targets employees who work with substances or conditions known to damage the skin. These programmes follow a planned schedule, include record-keeping, and trigger action when early symptoms appear. A routine GP check does not assess workplace exposure in this way, nor does it track changes over time linked to specific tasks. Early detection sits at the centre of skin health surveillance. When signs are identified early, employers can adjust tasks, implement controls, or provide treatment before the condition becomes chronic. This reduces absence, prevents long-term harm, and supports compliance with UK health and safety duties.
In high-risk industries, structured skin surveillance is used because exposure is frequent and often unavoidable. Sectors such as healthcare, manufacturing, cleaning, and construction involve regular contact with irritants such as detergents, solvents, and water. Without a formal system, early symptoms are missed, and cases are reported only when damage becomes severe. A structured programme creates consistency, accountability and clear intervention points.
Understanding Occupational Dermatitis
Occupational dermatitis is a skin condition caused or made worse by workplace exposure. It usually affects the hands but can spread to other areas depending on the level of contact. The condition develops over time through repeated exposure rather than a single incident. Common workplace causes include: chemicals such as solvents, oils, and cleaning agents; wet work where hands are in water or damp conditions for long periods; and frequent hand washing, especially without proper skin care. These exposures weaken the skin barriers, and once damaged, the skin becomes more vulnerable to further irritation and infection. There are two main types:
- Irritant contact dermatitis –
This is the most common form, and it occurs when substances directly damage the skin. Repeated exposure builds up the effect. Even mild irritants, when handled daily, can lead to visible damage. - Allergic contact dermatitis –
This develops when the immune system reacts to a specific substance. Once sensitised, even small amounts trigger a reaction. Common allergens include latex, certain metals, and preservatives in products.
Data from the Health and Safety Executive shows that thousands of new cases of work-related skin disease are reported each year in the UK, with contact dermatitis making up the majority. High-risk occupations continue to report the highest incidence, especially where control measures and surveillance are limited. Without early action, occupational dermatitis can lead to long-term skin damage, reduced work capacity, and, in some cases, a permanent job change. This makes prevention and early identification critical for both employees’ health and employer responsibility.
Why Skin Health Surveillance Matters for Employers
Skin health surveillance is not optional where there is a clear risk. UK law imposes a duty on employers to protect employees from harm arising from workplace exposure. Under the Health and Safety at Work etc. Under the 1974 Act and the Control of Substances Hazardous to Health Regulations 2002, employers must assess risks, apply control measures, and monitor health where exposure could lead to conditions such as occupational dermatitis. A structured skin surveillance programme helps you act early. Once dermatitis develops, recovery takes time, and repeated exposure often worsens the condition. In some cases, employees need to change roles or leave work entirely. Early identification avoids this outcome and supports long-term employee health.
There is also a direct business impact; work-related skin disease leads to absence, reduced performance, and higher staff turnover. Claims linked to occupational dermatitis carry financial and legal risks, especially when no monitoring or prevention system is in place. Data from the Health and Safety Executive continues to show that dermatitis remains one of the most common occupational diseases in the UK. Skin health surveillance supports productivity. Employees work more effectively when discomfort, irritation, or pain does not interfere with daily tasks. A clear system also shows commitment to well-being, which strengthens trust and retention across teams.

Who Needs Skin Surveillance in the Workplace?
Skin surveillance is required where employees are exposed to substances or conditions known to damage the skin. This applies across several high-risk industries:
- Healthcare
Regular washing of hands, glove use, and exposure to cleaning agents increase the risk. - Construction
Contact with cement, solvents, and adhesives often leads to skin irritation. - Manufacturing
Oils, chemicals, and repeated handling of materials affect the skin barrier. - Cleaning and facilities
Frequent use of detergents and disinfectants leads to prolonged exposure. - Hair and beauty
Hair dyes, shampoos, and chemical treatments create a high-risk environment.
Risk is not limited to the industry alone. Any role involving repeated exposure to irritants or allergens requires attention. This includes tasks involving wet work, chemical handling, or prolonged glove use. Employers must act when risk assessments identify potential for skin damage. Under COSHH, health surveillance becomes necessary when there is a reasonable likelihood of disease developing due to exposure. Waiting for symptoms to appear is unacceptable; a proactive approach ensures early detection, protects employees, and keeps your business compliant.
Signs and Symptoms of Workplace Dermatitis
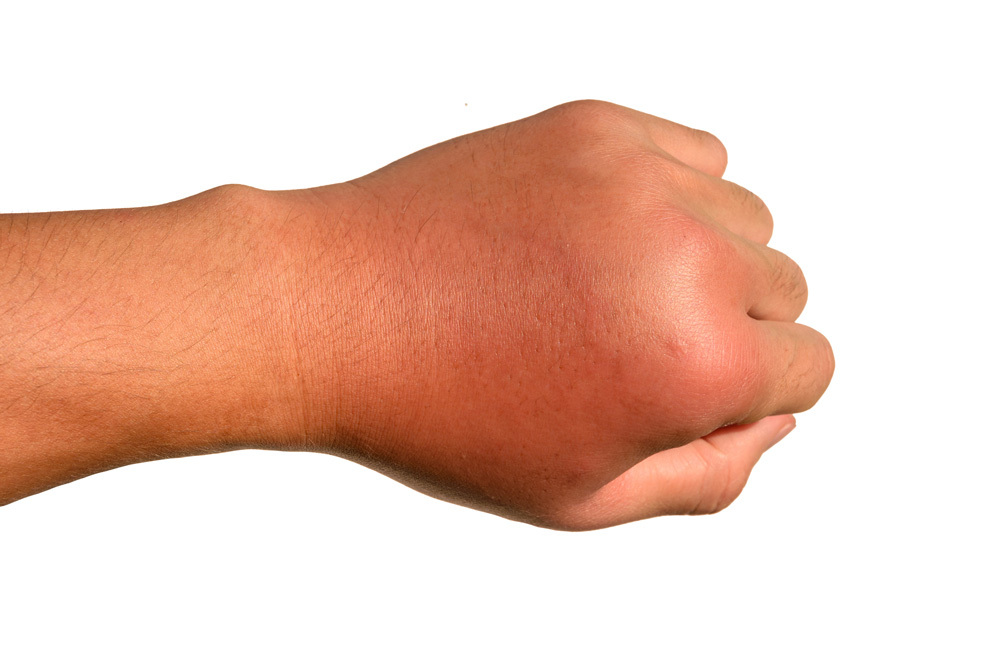
Workplace dermatitis does not appear suddenly in most cases; it builds over time, and the early signs are often mild enough to ignore. This is where many employees miss the warning stage. The first symptoms usually include dry or rough skin, redness, mild itching, or a feeling of tightness, especially on the hands. As exposure continues, the skin may start to crack, flake, or develop small blisters. In more advanced cases, it becomes painful, swollen, and prone to infection.
What makes this condition difficult to manage is how easily it goes unnoticed in the early stages. Employees often assume dryness is due to weather or routine hand washing, especially in roles where frequent cleaning is normal. In sectors like healthcare or cleaning, repeated exposure to water and chemicals is part of the job, so early irritation is seen as expected rather than a warning sign. This delay in recognising symptoms leads to cases being reported only when the condition starts interfering with daily work.
Early reporting is critical, and once the skin barrier is damaged, continued exposure makes recovery slower and increases the risk of long-term dermatitis. Guidance from the Health and Safety Executive highlights that early identification and intervention are key to preventing progression. Employees need to feel confident reporting even minor changes, and employers need systems in place to respond quickly.
The impact on day-to-day work is often underestimated. Simple tasks such as wearing gloves, handling tools, or washing hands become uncomfortable or painful. In some cases, employees reduce their productivity or avoid certain tasks altogether. Over time, this affects attendance, performance, and overall well-being. Without proper management, occupational dermatitis can lead to long-term absence or even the need to leave the role entirely.
What Happens During Skin Health Surveillance?
Skin health surveillance follows a structured process designed to track changes over time and identify early signs of damage. It starts with a baseline assessment. This is carried out when an employee begins a role or is first exposed to a risk. The skin condition is recorded at this stage, creating a reference point for future checks. Regular skin checks are then carried out at planned intervals, depending on the level or risk. These checks are often simple but consistent. Trained professionals look for visible signs such as redness, dryness, or cracking and compare their findings with previous records. This ongoing monitoring helps identify patterns before they become serious.
Employee questionnaires form an important part of the process. These allow individuals to report symptoms such as itching or irritation, which may not always be visible during a check. Many cases of dermatitis begin with discomfort rather than visible damage, so this step adds an extra layer of detection. All findings are recorded and monitored over time. This creates a clear history of skin health for each employee and helps employers identify trends across teams or roles. If changes are identified, action is taken early. This may involve reviewing control measures, adjusting tasks, or introducing additional protection.
Where symptoms suggest developing dermatitis, escalation is required. Employees may be referred for further occupational health assessment or medical advice. At this stage, the focus shifts from monitoring to intervention, ensuring the condition does not progress further. A structured approach like this keeps the process consistent, compliant, and effective across the workforce.
Workplace Dermatitis Prevention Strategies
Preventing workplace dermatitis starts with control, not treatment. Once the skin is damaged, recovery takes time, and repeated exposure makes the condition worse, so the focus must stay on reducing risk at the source. Risk assessments form the foundation. Employers need to identify substances and tasks which expose employees to irritants or allergens, then apply practical control measures. This includes substituting harmful chemicals where possible, limiting contact time, and introducing safer systems of work. Guidance from the Health and Safety Executive makes it clear that prevention must begin by eliminating or reducing exposure, rather than relying solely on protective equipment.
Personal protective equipment plays a role, but it needs to be suitable for the task. Gloves, for example, must match the type of substance being handled and should be used correctly. Prolonged glove use without breaks can also damage the skin, so this needs to be managed. PPE works best when combined with other controls, not used as the only line of defence. Safe handling of substances is another key area. Employees need clear instructions on how to use, store, and dispose of materials safely. Even common products like cleaning agents or hair treatments can cause damage when handled repeatedly without proper precautions.
Skin care routines often get overlooked, but they are a critical part of prevention. Providing access to suitable hand cleansers, moisturisers, and drying methods helps maintain the skin barrier. Harsh soaps or excessive washing without protection can increase risk, especially in roles involving wet work. Training and awareness tie everything together. Employees need to understand the risks, recognise early symptoms, and know when to report concerns. Without this, even the best control measures fail. Awareness creates consistency in how prevention is applied across the workplace.
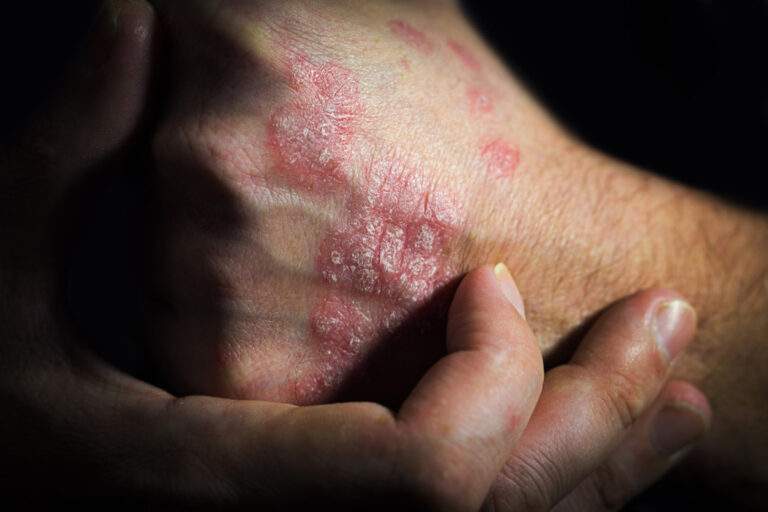
Employer Responsibilities for Dermatitis Prevention
Employers have a clear legal duty to protect employees from workplace exposure-related skin damage. Under the Control of Substances Hazardous to Health Regulations 2002, any substance which can harm the skin must be assessed and controlled. This duty begins with identifying risks. Employers must assess all substances and processes which may lead to occupational dermatitis, then implement measures to reduce or eliminate exposure. This is not a one-time exercise; risk assessments need regular review, especially when tasks, materials, or working conditions change.
Control measures must be practical and effective. This includes providing appropriate PPE, ensuring safe systems of work, and making suitable skin care products available. Employees should not be expected to manage these risks on their own. Training is also a legal requirement. Staff must receive clear guidance on how to handle substances safely, use protective equipment, and recognise early signs of skin damage. Without proper training, compliance becomes inconsistent and risk increases.
Record-keeping supports compliance and accountability. Employers need to maintain documentation of risk assessments, control measures, and any health surveillance carried out. These records provide evidence of action and help track whether existing controls are working.
Consequences of Ignoring Skin Surveillance
Ignoring skin surveillance leads, over time, to one outcome: an increase in occupational dermatitis cases. Without monitoring, early symptoms are missed, and employees continue to be exposed until the condition becomes more severe and harder to manage. This creates legal risk. The Health and Safety Executive has the authority to investigate and take enforcement action where employers fail to control exposure or monitor health appropriately. This includes improvement notices, fines, and in serious cases, prosecution.
The impact on employee health is long-term. Occupational dermatitis can become chronic, affecting an individual’s ability to work comfortably or safely. In some cases, employees need to change roles or leave their jobs entirely due to ongoing skin problems. There are also clear financial and operational costs, increased absence, reduced productivity, and staff turnover, all of which affect business performance. Compensation claims add further pressure, especially where there is no evidence of prevention or monitoring. Reputation is another factor; employers who fail to protect their workforce risk losing trust, both internally and externally. In industries where safety standards matter, this can affect recruitment, retention, and client confidence.
How Healthscreen UK Supports Skin Surveillance
At Healthscreen UK, skin surveillance is delivered as a structured, compliance-led service designed around your workplace risks. No two environments are the same, so the approach is built to reflect the substances your teams handle, the tasks they perform, and the level of exposure. You can choose on-site or clinic-based services. On-site assessments work well for larger teams or high-risk environments that require regular monitoring. Clinic appointments suit smaller teams or where flexibility is needed. Both options follow the same standard of care and reporting, ensuring consistency across your workforce.
Each programme is tailored, including setting the right frequency of checks, selecting appropriate assessment methods, and aligning everything with your existing risk assessments. The aim is simple: identify early signs of skin damage before they develop into occupational dermatitis, and act on them quickly. All assessments are carried out by qualified occupational health professionals who understand both clinical signs and workplace risks. This matters because recognising early symptoms is only part of the process; knowing when to escalate and what action to take is equally important.
Coverage is available across the UK, making it easier to manage multi-site operations without gaps in monitoring. Whether your teams are based in one location or spread across regions, the service remains consistent. Reporting is clear and compliance-focused. You receive structured records which support your COSHH duties, highlight any concerns, and provide a documented trail of action. This not only protects your employees but also your business.
Book Skin Surveillance for Your Workforce
If your employees are exposed to irritants, chemicals, or wet work, waiting for symptoms to appear is a risk you do not need to take. Early action keeps your workforce protected and your business compliant. Book a skin surveillance programme with Healthscreen UK and put in place a clear system to monitor, manage, and prevent occupational dermatitis. Speak to the team today to arrange your assessment and take control of workplace skin health before it becomes a problem.
FAQs
Q. What is skin surveillance in the workplace?
Skin surveillance is a planned process used to monitor employees who are exposed to substances or conditions which can damage the skin. It involves regular checks, simple questionnaires, and record-keeping to identify early signs such as dryness, redness, or irritation. The aim is to detect problems early and take action before they develop into occupational dermatitis. It is focused on workplace risks, not general health.
Q. Is skin health surveillance a legal requirement in the UK?
Yes, in situations where there is a clear risk. Under the Control of Substances Hazardous to Health Regulations 2002, employers must provide health surveillance when employees are exposed to substances known to cause skin disease. This applies when there is a reasonable chance of harm despite control measures. It forms part of an employer’s wider duty to protect health at work.
Q. How often should skin surveillance be carried out?
The frequency depends on the level of risk identified in your assessment. High-risk roles may require more frequent checks, especially in the early stages of exposure. In many cases, an initial baseline assessment is followed by periodic reviews at set intervals. If any symptoms are reported, checks may need to be performed more frequently. A consistent schedule is important to track changes over time.
Q. What industries are most at risk of occupational dermatitis?
Industries with regular exposure to irritants or allergens carry the highest risk. This includes healthcare, construction, manufacturing, cleaning and facilities, and hair and beauty. Roles involving wet work, chemical handling, or frequent hand washing are particularly affected. Data from the Health and Safety Executive shows that these sectors continue to report higher levels of work-related skin disease.
Q. How can workplace dermatitis be prevented?
Prevention starts with identifying and controlling exposure. Employers need to carry out risk assessments, reduce contact with harmful substances, and introduce safe systems of work. Suitable PPE should be provided where needed, along with proper training on its use. Skin care also plays a role; access to appropriate cleansers and moisturisers helps maintain the skin barrier. Most importantly, early signs should be reported and acted on without delay.